
Funded by the WITH Foundation

Grief and Loss
Katy Stratigos, MD, Lauren R. Charlot, PhD, LICSW , and Andrea Caoili, LCSW
Contents
Fundamentals of Psychopharmacology
The Lived Experience Perspective
- Communicating with Patients with IDD and Their Family Members
- Considerations for Waiting Rooms
- Sensory Considerations for Medical Providers
- Cultural Competency and Prescribing
Psychiatric Assessment Considerations
Medical Assessment Considerations for Patients with IDD/MH
Best Practices in MH Diagnosis and Treatment
- Trauma and Stressor Related Disorders
- Anxiety Disorders
- Obsessive Compulsive and Related Disorders
- Depressive Disorders
- Bipolar Disorders
- Grief and Loss
- Schizophrenia and Other Psychotic Disorders
There is an extensive body of research that focuses on the relationship among grief, bereavement and mood disorders. Unfortunately, many clinicians assessing and treating individuals with Intellectual and Developmental Disabilities (IDD) and Autism Spectrum Disorder (ASD) may not be familiar with this body of work. In addition, few studies focus on grief and grief work in people with IDD. This section will investigate the many faces of grief and outline appropriate treatment techniques and resources.
DSM-51 Changes to Assessment and Diagnosis of Bereavement
The authors of the DSM-5 eliminated the longstanding concepts that defined the boundaries between bereavement and Major Depressive Disorders (MDD). In previous editions of the DSM, the diagnosis of bereavement, rather than MDD, required that depressive symptoms occurred in the context of significant losses, regardless of whether the depressive symptoms met the criteria for major depression.
The DSM-5 requires clinical judgment as to whether the severity and symptoms in response to loss rise to the level of a major depressive episode. The issue involves discriminating between the factors that increase the likelihood that significant loss triggers MDD and not other DSM-5 disorders. Persistent Complex Bereavement Disorder in the DSM-5 presents as an intense, turbulent, intrusive, prolonged, and maladaptive process.
Criteria for Persistent Complex Bereavement Disorder
- Lasts at least 6 months for children and 12 months for adults
- Manifestations of separation distress, traumatic distress
- Significant functional impairment
Grief is a normal part of life
Grief as a result of loss is experienced by all people at some point in their lives. A wide variety of losses may impact a person including loss of pets, home, family members, employment and other things that make up a person’s identity. Kubler-Ross2 developed a five-stage model of grief to describe the different stages and experiences of a person when bereaved. Later, Kessler3 amended the model to include a 6th stage, meaning. People do not follow each stage independently from the other, rather they pass through phases fluidly based on their emotional and physiological state.
Figure 1. 5 Stages of Grief Model
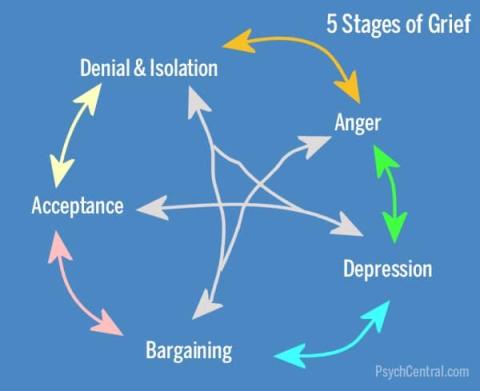
Image source: https://psychcentral.com/lib/the-5-stages-of-loss-and-grief/
Table 1. Six Stage Model of Grief (Kubler-Ross, Kessler)
|
Stage |
Description |
|
Denial |
Numbness, "it’s a mistake", false hope |
|
Anger |
Frustration, irritability, blaming others: "Why me?", 'it's not fair! |
|
Bargaining |
"If I only did ...", "What if" |
|
Depression |
Emptiness, feeling overwhelmed, possible suicidal thoughts |
|
Acceptance |
Emotions stabilize, new reality, more good days than bad |
| Meaning | Finding peace and hope for the future |
Considerations for patients with IDD
As with other stressful life events, the impact of personal loss may be underestimated in individuals with IDD. Access to interventions is undermined by misconceptions that people with IDD do not understand death and need to be “protected” from facing emotional experiences. As a result, people with IDD may not be told of deaths in a timely fashion or not permitted to go to a funeral out of concern they will “get upset.” As a result of these biases, people with IDD may not be permitted to grieve with their family, attend funerals or memorial services, or provided psychological supports to cope with the loss. A poignant example involves the person waiting or searching for the deceased, not fully understanding that death is irreversible. Such responses, when an individual is not involved in family rituals, may create more distress for other grieving family members and have systemic effects on the survivors.
The other potential complications that implicate misdiagnosis are the underuse of grief counseling and the overuse of ineffective treatments. For example, developmental features can cloud the presentation of a person’s response to loss such that separation anxiety, severe withdrawal, aggression or self-injury are considered symptoms of another condition. This mischaracterization can result in the person receiving treatment (including medications to treat different conditions) that is not indicated for grief.
People with IDD have a lifetime of loss and devaluing experiences such as decreased contact and/or inability to live with family, friends, and other natural supports. They may also experience the loss of meaningful work, their home, and housemates, all of which have a significant impact. A major loss like the death of a parent, relative, friend or caregiver occurs in the context of multiple other losses, becoming “the straw that breaks the camel’s back.” Unrecognized or undiagnosed grief may result in inadequate grief resolution and put the person at greater risk of Persistent Complex Bereavement Disorder. In this sense, grief resembles untreated trauma in terms of its transformation into a disorder that is more complex and difficult to treat.
The grief response for people with IDD can be a prolonged process that contributes to a decline in cognitive, social and emotional presentation. There is a tendency to misattribute many emotional and behavioral features of an evolving grief response to major forms of psychopathology. The expression of grief also follows a developmental trajectory and depends in part on age, cognitive and adaptive abilities, communication skills, and a host of other psychosocial factors, all of which shape a person’s response to loss. In many cases, the expression of externalizing behavioral symptoms overshadows emotional responses and the recognition of grief as a root cause is under-appreciated.
Table 2. Emotional and Behavioral Symptoms of Grief in IDD
|
Emotional symptoms |
Behavioral symptoms |
|
|
Grief responses related to crises other than death may also be significant and require clinical attention. Individuals with IDD, and particularly some with ASD, experience significant health, emotional and behavioral challenges secondary to loss other than death. Many people with IDD lack control and ability to make choices regarding their living arrangements, jobs, social opportunities and even their medical and psychiatric care. Lack of control and choice likely amplifies anxiety in many contexts. The 2019-2020 advent of the COVID-19 virus and related restrictions such as needing to shelter in place provide an extreme example of this form of loss and its impact on the lives of people with IDD.
Effective psychosocial treatment options for people with IDD
The few large-scale scientific studies available have not helped to guide many clinicians seeing patients with IDD who experience grief, and in many circumstances, interventions known to be effective with other populations are extrapolated. For example, preventative or proactive interventions may take advantage of frequent, less extreme situations to help the individual learn how to cope with loss and change. These strategies may translate into greater resilience by preparing people for later, more significant losses. Giving the person with IDD choice and opportunities to be part of natural grieving, funerals and other religious and social responses to death is an important and necessary intervention. For bereaved adults with IDD, informal tactics include such activities as an acknowledgment of loss, supportive listening, involvement in rituals, memorialization, bibliotherapy, addressing spiritual beliefs, and life story work along with concrete related activities. At the formal level, it has been reported that attachment work, addressing coping mechanisms, and guidance and education of home staff, as well as coordination with home staff, have been successful.” Group supports and planned activities may also be effective, including visits to funeral homes, making memory tables, and “comfort bags.”
Bereavement counseling can benefit individuals with IDD, including the full range of levels of severity, regardless of the length of time since death. There are adapted, manualized grief counseling resources available.
When does bereavement require psychopharmacological intervention?
Psychopharmacological intervention may be beneficial for some people with IDD in conjunction with individual and/or group psychotherapy. When the bereaved person with IDD meets the criteria for clinical depression, has significant impairment in daily functioning and/or is experiencing suicidal ideation, antidepressant therapy may be appropriate.
Case Vignette
George is a 60-year-old man with mild ID and autism. Record review indicated poorly supported diagnoses of bipolar disorder and schizophrenia diagnosed in 2017. George lived at home with his younger brother and parents for his entire childhood. His mother homeschooled him although his brother went to public school. George’s entire immediate family has always been very close and involved in caring for and supporting George. His father died when he was 16 years old, and his brother moved out of the family home when he turned 18 and went to college. This left only George and his mother living in the family home for many years until his mother passed in 2016. At that time, George moved to a group home. Although he still has some support from his brother, his brother does not live in the same state and travels a lot for work.
Before moving to the group home, George attended a day program five days per week. He also received occasional weekend respite and was involved in his church. His primary care manager was a long-time family friend, but he retired shortly before the passing of George’s mother. Upon moving to the group home, new primary care services needed to be established.
George was referred for psychiatric assessment at an IDD specialty clinic in 2018 due to "aggressive behaviors," limiting his day program to only twice/week. His sleep was disrupted, with awakening often in the middle of the night. He appeared irritable and would cry frequently. Upon assessment and symptom tracking, it was noted that George often spoke about his childhood and his family. When he did speak of his parents and his “old life,” as he called it, he would cry. This often led to self-injury (hitting himself on the head, chest, and thighs), yelling and property destruction. Occasionally, it escalated to physical aggression.
Taking symptom trends into consideration, it was determined that a diagnosis of complex bereavement disorder should be considered. In-home supports were coordinated with the group home to provide additional assistance to titrate George off ineffective medications and begin a trial on an SSRI. In addition to psychopharmacological treatment, George was screened and then enrolled in bereavement-focused psychotherapy.
1 American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders (5th ed.). Washington, DC: American Psychiatric Association, 2013.
2 Kubler-Ross, E. On Death and Dying. New York, NY: Collier Books/Macmillian, 1969.
3 Kessler D. Finding Meaning: The Sixth Stage of Grief. New York, NY: Scribner, 2019.
References
American Psychiatric Association. (2013). Diagnostic and statistical manual of mental disorders (5th ed.). Arlington, VA: Author.
Bonell-Pascual, E, Huline-Dickens, S, Hollins, S (1999). Bereavement and grief in adults with learning disabilities: A follow-up study. British Journal of Psychiatry. 175(4):348–350.
Brickell, C, Munir, K. (2008) Grief and its complications in individuals with intellectual disability. Harvard Review of Psychiatry. 16(1): 10-12
Clements P, Focht-New, G, Faulkner, M.(2004). Grief in the shadows: Exploring loss and bereavement in people with developmental disabilities. Issues in Mental Health Nursing. 25: 799-808.
Clute, MA. (2010). Bereavement interventions for adults with intellectual disabilities: What works? Omega (Westport).61(2):163-77.
Clute, M. (2017) A grounded theory study of the bereavement experience for adults with developmental disabilities following the death of a parent or loved one: Perceptions of bereavement counselors [PhD dissertation]. Cleveland, OH: Case Western Reserve University.
Dowling, S., Hubert, J., White, S., & Hollins, S. (2006). Bereaved adults with intellectual disabilities: a combined randomized controlled trial and qualitative study of two community‐based interventions. Journal of Intellectual Disability Research, 50(4), 277-287.
Fletcher, R. I., Barnhill, J., Cooper, S. (2017). Diagnostic Manual-Intellectual Disability (DM-ID-2): A textbook of diagnosis of mental disorders in persons with intellectual disability. Kingston, NY: NADD.
Hume, K, Regan, T, Megronigle, L, & Rhinehalt, C. (2015). Supporting students with autism spectrum disorder through grief and loss. Autism at a Glance Brief. 48(3): 128-136
MacHale, R, Carey, S. (2002). An investigation of the effects of bereavement on mental health and challenging behavior in adults with learning disability. British Journal of Learning Disabilities. 30(3):113–117.
Mosher, PJ. (2018). Everywhere and nowhere: Grief in child and adolescent psychiatry and pediatric clinical populations. Child Adolescent Psychiatry Clinics of North America. 27(1):109-124.
Shear, M. K., & Bloom, C. G. (2017). Complicated grief treatment: An evidence-based approach to grief therapy. Journal of Rational-Emotive & Cognitive-Behavior Therapy, 35(1), 6-25.
Van Dyke, L. (2003) Lessons in Grief & Death: Supporting People with Developmental Disabilities in the Healing Process. Homewood, IL: High Tide Pr
